Are Granulomas Cancer?
Granulomas are rarely malignant. Tissue sampling, or a biopsy, done during surgery can tell whether a granuloma is cancerous or not.
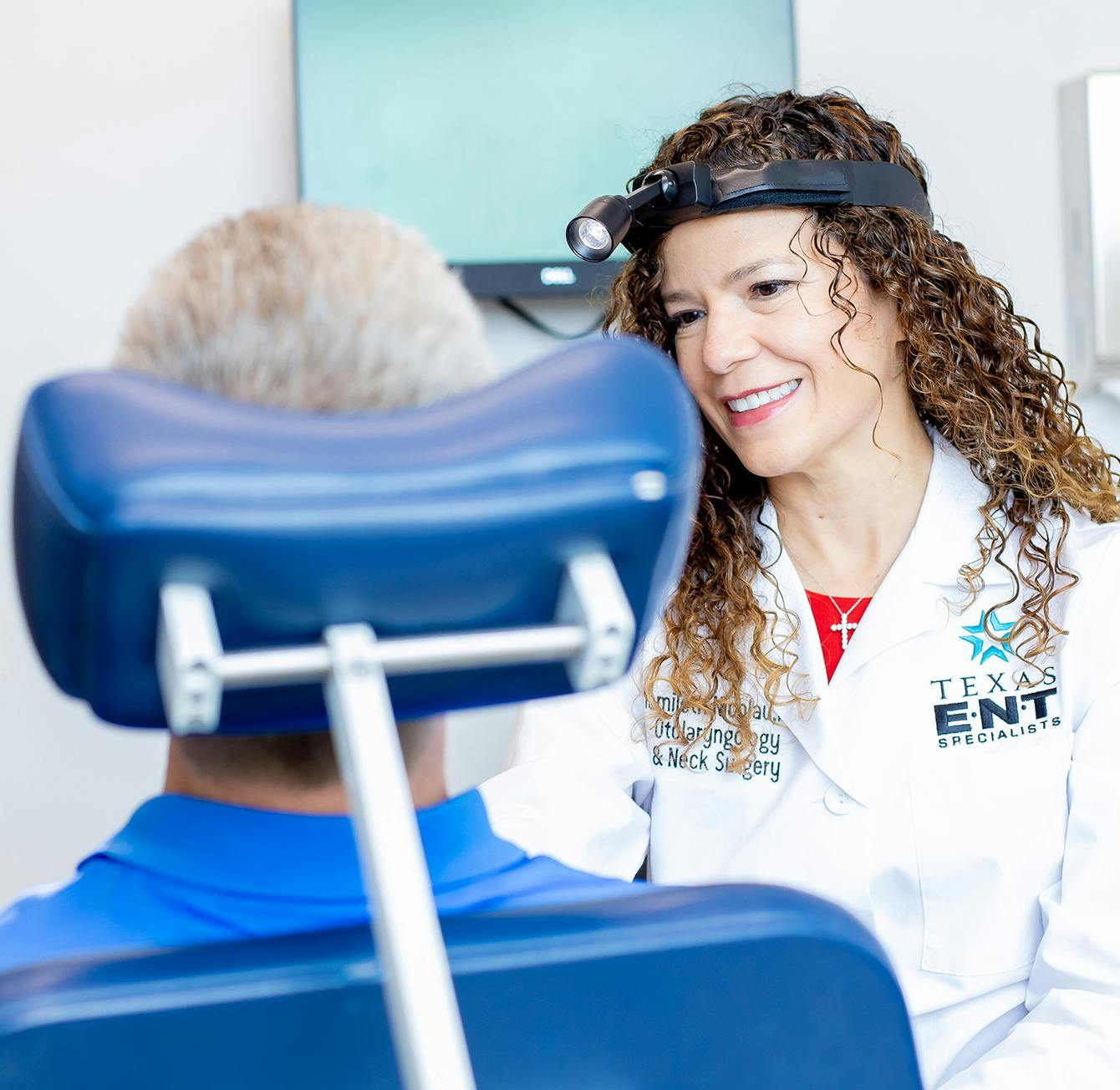
Vocal cord paralysis can be caused by neck or chest surgery, by benign or malignant growths near the nerve to the vocal cord, by bacterial or viral infections, by certain types of chemotherapy, or by trauma. The trauma may be a neck trauma, a blunt injury to the larynx, or caused by a breathing tube. The vocal cords normally open wide when you breathe to let air into your lungs, and then they come to the midline when you speak in order to compress the air flowing from your lungs and cause high frequency vibration of their cover. It is this vibration that makes the sound waves that create the base for your voice.
